
Lyme disease
What is Lyme disease?
Symptoms of Lyme disease
Early diagnosis and treatment of Lyme disease is crucial
Late-stage chronic Lyme disease
Lyme disease and denial
Vitamin D resistance
Prevention / remedies / cures / treatment of late-stage Lyme disease
References
What is Lyme disease?
Lyme disease is a bacterial infection obtained from a tick bite. It is the most common in North America and Europe, but it exists all over the world in places where there are ticks.
It is the leading vector-borne disease in America, with an estimated 40 million undiagnosed sufferers. Some doctors who are properly familiar with Lyme estimate that a third to a half of all people presenting to them are infected with Lyme disease. It is possible to be infected and show few or insignificant symptoms.
The bacterium which causes Lyme disease in the USA is Borrelia burgdorferi. Outside North America and Europe, B. garinii and B. afzelii are more common. When a tick carrying this bacterium bites a person, they may become infected if the bacteria in the tick get the opportunity to enter the bloodstream through the bite. It is very important if you are bitten by a tick to remove it properly without squeezing it, and to disinfect the tick bite immediately. See how to deal with a tick bite.
Borrelia burgdorferi is a spirochaete type bacteria similar to those that cause syphilis (Treponema pallidum), leptospirosis (Leptospira interrogans) and stomach ulcers and digestive problems (Helicobacter pylori).
B. burgdorferi is most associated with arthritis;
B. garinii is most associated with neurological symptoms;
B. afzelii are associated with and skin rashes and other skin disorders.
However, these associations are not absolute.
Symptoms of Lyme disease?
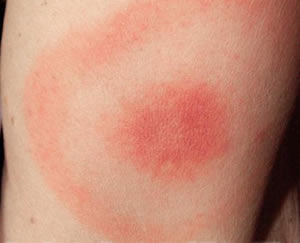
- Rash around the tick bite (Erythema Migrans rash).
- Fever and chills.
- Fatigue.
- Body aches.
- Headaches.
- Frequent urination.
- Interstitial cystitis - recurring pain in the bladder and surrounding pelvic region.
- Stiff neck.
- Pain. Joint pain, bladder and pelvic pain, and general pain around the body.
- Neurological issues. Lyme disease is a root cause of multiple sclerosis, Parkinson's, Alzheimer's, Lou Gehrig's diseases and many other brain and nervous disorders. (1, 3, 6, 11)
- Atherosclerosis. Bacterial infections are a cause of damage to and inflammation of blood vessels.
- Heart disease.
- Arthritis.
- Liver inflammation.
- Inflammation of the eyes.
- Chronic fatigue.
- Brain fog.
- Fibromyalgia.
Early / initial symptoms
Classic symptoms
Late-stage symptoms
Early diagnosis and treatment of Lyme disease is crucial
Generally throughout Grow Youthful I am totally against the use of antibiotics. However, antibiotics have a place in the case of life-threatening or dangerous bacterial infections. If you diagnose Lyme disease early in its progress, it is relatively easy to treat with a course of an antibiotic such as doxycycline.
The Lyme disease spirochete is capable of survival in a host for prolonged periods of time, hiding in a biofilm or apparently commensal (harmless). Some patients with Lyme borreliosis may require more than the currently recommended two to three week course of antibiotics to eradicate strains of the spirochete which grow slowly. (10) It is capable of morphing into different forms and structures, including cysts.
Only early-stage Lyme disease is recognised by the American health insurance industry, American health and medical boards, and nearly all conventional Western medical doctors.
Without early treatment, Lyme disease can become a debilitating ailment lasting for many months, years or even remainder of life.
Late-stage chronic Lyme disease
If symptoms persist after the first course of antibiotics lasting 3 to 4 weeks, most conventional doctors refer to this as Post-treatment Lyme Disease Syndrome (PTLDS). They argue that the lingering symptoms are due to damage to tissues and the immune system that occurred during the infection.
Late-stage Lyme disease is often not diagnosed, or misdiagnosed. If Lyme disease is allowed to progress, the Borrelia bacteria:
- Form biofilms that protect the bacteria.
- Morph into different forms, including cysts and non-spirochaete.
- Increasingly become antibiotic-resistant.
- Co-infect cells along with other bacteria and viruses.
- Bypass the standard Lyme infection tests done by conventional doctors, so it looks like the patient is not infected.
- Bypass the blood-brain barrier by burrowing through it with their spirochaete shape, so infecting the brain and central nervous system.
- Cause late-stage symptoms that are difficult to connect to the initial infection.
Lyme disease and denial
Conventional pharmaceutical medicine does not have any cure for late-stage Lyme disease.
Doctors are only taught about early-stage Lyme disease, they are not taught about the late-stage Lyme disease so many of them deny that it exists. Instead, they look for other causes and misdiagnose their patients. Their denial looks as if it is justified because the patient's tests often come back negative.
Patients with late-stage Lyme disease usually suffer pain, fatigue, debilitation and a variety of serious ailments for many years, going from doctor to doctor while hoping that one will eventually diagnose their illness. Sometimes they lose their livelihood, their families, their homes, and become destitute in the process.
Doctors who correctly diagnose late-stage Lyme disease risk losing their medical licence. Even though they have been successful in treating many of their patients, they risk the ire of their medical boards, health insurance companies, pharmaceutical companies, and bodies upon which they may depend for their professional progress.
Lobbying (bribes, threats, corruption) by the American health insurance industry has brought about this situation, because late-stage Lyme disease is a financial disaster for the health insurers. Conventional medicine has no treatment, so late-stage Lyme disease must be managed for years or even the rest of the patient's life. The insurance industry prefers to classify late-stage sufferers as malingerers or having psychological issues, and deny them cover.
With more than forty million people in America suffering from Lyme disease, if it was diagnosed correctly and treated with conventional and pharmaceutical medicine, the profits of the health insurance industry would suffer.
Vitamin D resistance
Several bacteria, especially spirochete bacteria like those that cause Lyme disease, also cause what I call vitamin D resistance. These bacteria cause a decrease in the efficiency of vitamin D receptors by 60 to 80 times. This means that someone diagnosed with Lyme disease can have a blood test that shows a normal level of vitamin D, but at a cellular level is suffering from a severe vitamin D deficiency. (12)
Several other bacteria like Chlamydia and Mycoplasma, some viruses, and some moulds like Aspergillus, also cause this breakdown in the efficiency of vitamin D receptors.
Supplementing vitamin D will not remedy vitamin D resistance. Instead, what is required is to increase the efficiency of vitamin D receptors. See remedies below.
Prevention / remedies / cures / treatment of late-stage Lyme disease
If you use any of these remedies, please come back next week (or whenever you have an outcome) and let us know about your experience. Please leave a comment as many people are interested.
See details of remedies recommended by Grow Youthful visitors, and their experience with them.
Doctors who have chosen to ignore the corruption have had some success using long courses of powerful pharmaceutical antibiotics. Unfortunately, even short courses of antibiotics can have lifelong negative consequences, as detailed here. Long courses of powerful pharmaceutical antibiotics are almost certain to cause a variety of horrible negative side-effects.
Natural treatment options for late-stage chronic Lyme disease are often more effective than antibiotics and other pharmaceutical prescription medications.
The treatment is conducted on several fronts:
- Biofilms must be dissolved and removed.
- Natural antibiotics may be more successful than pharmaceutical antibiotics, to which the Borrelia have acquired some degree of resistance.
- Everything possible must be done to enhance and support the immune system.
For most people, late-stage symptoms or PTLDS symptoms disappear after a few months.
- Diet. Eliminate sugar and refined carbohydrates. Try a ketogenic diet for a month. I strongly recommend the carbohydrate concentration approach to eating, discussed in detail in the Grow Youthful book.
- Gum turpentine. A powerful antimicrobial which can also remove biofilms.
- Vitamin D sufficiency and efficiency. The following will help improve vitamin D response (efficiency): (12)
Zinc, magnesium and boron sufficiency.
Eliminating seed oils from the diet.
Quercetin, which is found in onions, especially red onions. The richest food source is capers.
Omega-3 oil sufficiency.
Intense exercise bouts (if it is possible to do this in a healthy manner without risking injury).
TUDCA bile salts.
Resveratrol. - Coconut oil. (7, 8, 9)
- Borax.
- Oral hygiene, treat teeth and gums. Get tooth decay and periodontitis and gum infections treated. The mouth is a major source of microorganisms that infect the rest of the body, and can cause heart disease, dementia (including Alzheimer's), and numerous other serious ailments. (1)
- Oil pulling. An excellent daily or even weekly practice that removes pathogenic bacteria from the mouth.
- Iodine. (8)
- Herbs. The most effective herb to use is Chinese skullcap (or Huang Qin). Its botanical name is Scutellaria baicalens and it is a member of the mint family. It is used in Chinese and Japanese medicine. It contains the compounds baicalein and trihydroxyflavone. (5, 6, 7)
Baicalein is also found in Indian trumpetflower (Oroxylum indicum). (7)
Blue skullcap Scutellaria lateriflora has some similar properties and components.
Other herbs to use include Andrographis, Cat's Claw, Sarsaparilla. - Cranberries have the ability to break down biofilm. (2)
- Garlic. A powerful natural antibiotic, antiparasitic and fungicide.
- Probiotics.
- Rest and deep regular sleep.
- Stress management.
- Exercise. Regular exercise boosts the amount of oxygen circulating in the body, which acts against the Lyme bacteria.
- Turmeric.
- Cinnamon.
References
1. Deborah K. Shoemark, Shelley J. Allen.
The Microbiome and Disease: Reviewing the Links between the Oral Microbiome, Aging, and Alzheimer's Disease.
Journal of Alzheimer's Disease 43 (2015) 725-738. DOI 10.3233/JAD-141170.
2. Steinberg D, Feldman M, Ofek I, Weiss EI.
Cranberry high molecular weight constituents promote Streptococcus sobrinus desorption from artificial biofilm.
Int J Antimicrob Agents 25, 247-251.
3. MacDonald A B.
Alzheimer's disease Braak Stage progressions: reexamined and redefined as Borrelia infection transmission through neural circuits.
Med Hypotheses. 2007;68(5):1059-64. Epub 2006 Nov 17. PMID: 17113237.
4. Miklossy, Judith.
Alzheimer's disease - a spirochetosis?
Neuroreport. 1993 Jul;4(7):841-8.
5. MacDonald A B.
Plaques of Alzheimer's disease originate from cysts of Borrelia burgdorferi, the Lyme disease spirochete.
Med Hypotheses. 2006;67(3):592-600. Epub 2006 May 3. PMID: 16675154.
6. Judith Miklossy.
Alzheimer's disease - a neurospirochetosis. Analysis of the evidence following Koch's and Hill's criteria.
Journal of Neuroinflammation. 20118:90. DOI: 10.1186/1742-2094-8-90. Published: 4 August 2011.
7. A. Goc, A. Niedzwiecki, M. Rath.
In vitro evaluation of antibacterial activity of phytochemicals and micronutrients against Borrelia burgdorferi and Borrelia garinii.
J Appl Microbiol. 2015 Dec; 119(6): 1561-1572. Published online 22 November 2015. doi: 10.1111/jam.12970. PMCID: PMC4738477.
8. A. Goc, A. Niedzwiecki, M. Rath.
Cooperation of Doxycycline with Phytochemicals and Micronutrients Against Active and Persistent Forms of Borrelia sp.
Int J Biol Sci 2016; 12(9):1093-1103. doi:10.7150/ijbs.16060.
9. Sung Woo Jung, Sang Woo Lee.
The antibacterial effect of fatty acids on Helicobacter pylori infection.
Korean J Intern Med. 2016 Jan; 31(1): 30-35.
Published online 28 December 2015. doi: 10.3904/kjim.2016.31.1.30. PMCID: PMC4712431.
10. Alan B MacDonald, Bernard W. Berger, Tom G. Schwan.
Clinical implications of delayed growth of the Lyme borreliosis spirochete, Borrelia burgdorferi.
Acta Tropica, 48(1991)89-94. Elsevier ACTROP 00084.
11. Itzhaki Ruth F, Lathe Richard; Balin Brian J, Ball Melvyn J, Bearer Elaine L, Bullido Maria J, Carter Chris; Clerici Mario; Cosby S. Louise, Field Hugh, Fulop Tamas, Grassi Claudio, Griffin W. Sue T, Haas Jurgen, Hudson Alan P, Kamer Angela R, Kell Douglas B, Licastro Federico, Letenneur Luc, Lovheim Hugo, Mancuso Roberta, Miklossy Judith, Lagunas Carola Otth, Palamara Anna Teresa, Perry George, Preston Christopher, Pretorius Etheresia, Strandberg Timo, Tabet Naji, Taylor-Robinson Simon D, Whittum-Hudson Judith A.
Microbes and Alzheimer's Disease.
Journal of Alzheimer's Disease. Published online 8 March 2016. doi:10.3233/JAD-160152.
12. Mangin M, Sinha R, Fincher K.
Inflammation and vitamin D: the infection connection.
Inflamm Res. 2014 Oct;63(10):803-19. doi: 10.1007/s00011-014-0755-z. Epub 2014 Jul 22. PMID: 25048990; PMCID: PMC4160567.
